Nights and Weekends (and Holidays) in the ER
It's just not the same as weekdays. Our patients and staff deserve better.

I recently wrote about what I consider one of the greatest healthcare divides in America, which is the inequality of rural vs urban care. (The link is at the bottom; it was two posts ago.)
I admit that it’s not exactly that simple (for instance you can’t reasonably have every specialty at every hospital due to volumes). But it’s still not the same and getting worse. In my post I advised summer travelers to know where healthcare facilities were as they crossed our great land. I still believe that folks should be particularly thoughtful if they have a history of complex medical problems and suddenly find themselves in, for instance, South Moose, Idaho with a flare-up of their complicated seizure disorder and are roughly 150 miles from a gas station, much less a neurologist. (But actually quite close to a moose.)
However, another problem in healthcare comes to mind lately. And that is the hard reality that overnight, and on weekends, many things aren’t available that are during the weekday. (Just to be clear, holidays are exactly the same and sometimes worse…especially the holidays that cross weekends, involve the closure of physician offices on Friday or Monday and are particularly alcohol fueled.)
I will preface this by saying that this is a huge problem; in part because nights in the ER are not what they once were. This is year 31 since I finished my residency training. While there were always busy nights in the ER, especially in urban centers, smaller hospitals were often very slow. When I started my career in emergency medicine, our community ER would often be empty from about 0300 to 0700. I would go to our call-room in the middle of the night, lie down and the next thing I heard was the knock on the door from the day-shift doctor saying, ‘hey man, go home!’ That was true in many hospitals.
But things have changed and dramatically. Now, the night is nearly as busy as the day; sometimes more. Going into a night shift, whatever one’s job in medicine, is a thing that provokes no small amount of anxiety; and exhaustion. A glance across the desks of physicians, NPs and PAs and nurses will reveal a cornucopia of caffeinated beverages including exotically named energy drinks with obscure flavors (and contents of questionable health and utility). Not to mention a wide variety of snack food, all meant to keep the boilers going through the long watches of the night when everyone would really prefer to sleep.
(Well, not everyone would rather sleep. There are physicians, nurses and others who are happily nocturnal; and there are patients who resemble our friend the opossum…here’s an old reflection I wrote on the topic….https://edwinleap.com/the-big-possums-walk-the-night/)

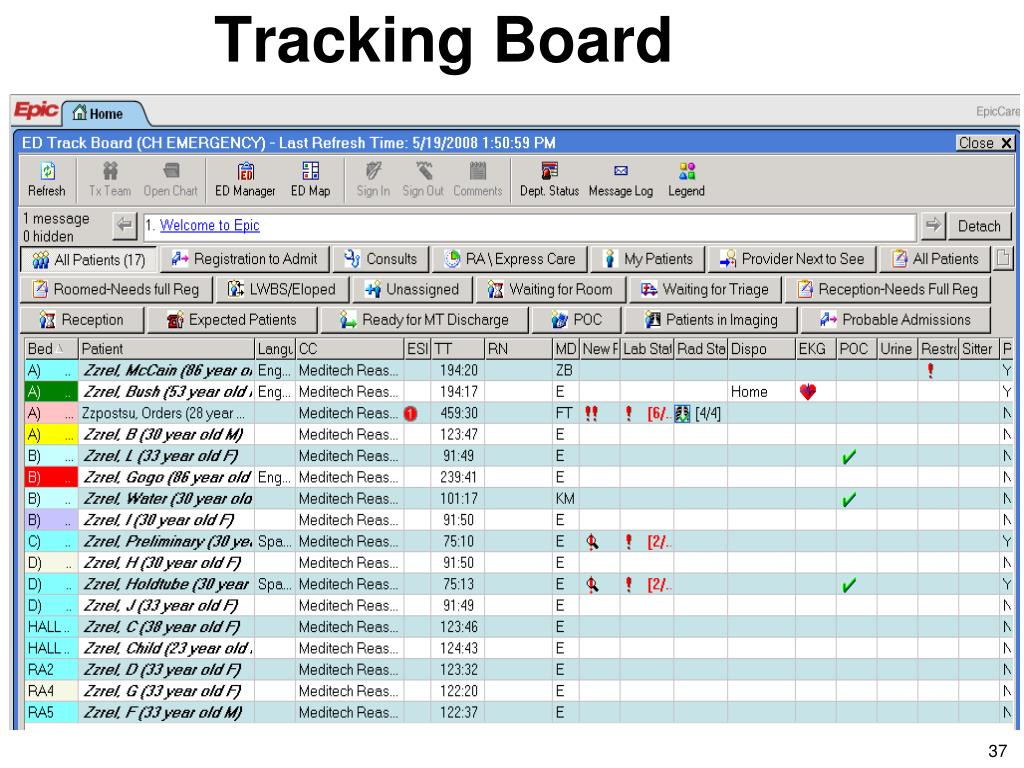
In these days of electronic medical records, our emergency departments frequently have large tracking-boards that gleam over our work stations. One of the first things a physician, nurse, secretary or other species does upon arriving to work is look up at that shining beacon of colored symbols in order to get a sense of how to gird his or her loins for the next eight to twelve hours.
Part of the problem is that those boards often display patients who are ‘on hold.’ That is, they are admitted but there is no available bed for them to go from the ER to an inpatient room. This is often tied to inadequate nurse staffing. Also, during the week open beds are held for surgery cases, which make more money for the hospital.
And obviously almost nobody in the hospital gets discharged at night. Families aren’t available and it would just be very complicated. During the weekend, discharges are also rare. The bottom line being that nobody leaves. The beds on the inpatient side remain full, so with the pipe full on the end, the flow of patients backs up in the ER.
But it’s really more than that. Discharges also are held up because many patients in the hospital need to go to nursing homes or rehab facilities; and there aren’t nearly enough to keep pace with our aging and very sick population. And when there are, the hospital often lacks night time or weekend social workers/case management workers to do the complex, form-heavy work of making those things happen. Furthermore nursing homes usually have diminished staff on nights or weekends.
Sorry, that was a lot of background!
So let’s circle back. The night time/weekend ER fills up with patients. And to return to the issue of the pipeline, the patients back up further into the waiting room where they may be treated from start to finish in the triage area.
The night team or weekend team will therefore come to work with perhaps dozens of patients holding, dozens of patients waiting, many of them very (and not unreasonably) annoyed. And there is no actual physical space to do much of anything. This is why wait times can be six, eight, twelve or more hours to be seen, treated and discharged for even minor issues.
This is bad enough. However, nights and weekends have traditionally been viewed as slower times, so hospitals and staffing companies treat them that way. There is little to no impetus to increase the number of physicians, nurses or others working nights. Nor is there any desire by specialists to be available on weekends when they aren’t being paid on-call fees by the hospital administration.
However, things are not the same as they were 30, 20 or even five years ago. Our patients can’t find primary care physicians and if they do often can’t afford to go to them. (As I’ve said they often can’t find dentists or obstetricians or other important professionals either.) Many times they can’t get their medications because their pharmacy is closed.
Our population is aging rapidly. Seniors are also caught in a terrible trap; we can do enough to help them survive dangerous medical events like stroke or heart attack, but we don’t do a great job of returning them to normal function. They are often in the ER for flare-ups of their chronic medical problems. And because our population is also aging alone, they are sometimes in the ER simply because they are scared; scared of falls or scared of death. (This is perhaps one of the most important things we offer them; simple reassurance.)
Overnight and on weekends those patients in need of placement in psychiatric or addictions facilities are stuck as surely as those needing nursing homes. We have an exploding population of patients addicted to fentanyl and methamphetamine. We have a tidal-wave of old and young alike with diagnoses of mental illness. Those in need of inpatient care for such problems, on nights or weekends, often have to endure the lights and noise until the world returns to some normalcy on Monday morning.
And much of this chaos arrives at night or after 5pm on Friday. In some cases because people work all day and can’t go to a physician any other time. In other, as with drugs and mental illness, because they simply have no markers of time and because bad things happen at night; like violence, overdose and car-crash.
To make matters worse, it isn’t at all unusual to find that particular tests or interventions can’t be done until the next day; or the next Monday. Particular specialists might not be available, psychiatrists, ophthalmologists, oncologists, urologists or others depending on the size of one’s hospital. MRI or ultrasound, nuclear medicine tests, physical therapy evaluations, cardiac stress tests can be delayed. Particular surgeries may have to wait unless truly emergent. Patients who could be treated and discharged from the hosptial may have to wait two or three days until the bright light of Monday morning returns healthcare to normalcy.
I remember once being told that a neurologist wouldn’t be available after 5 pm, and I thought, ‘well that makes sense, after people never have strokes at night, right?’
For some reason we seem to labor under an old paradigm of medicine, in which people had their own physicians to see for regular problems, the hospital wasn’t a 24/7 refuge as it is now, and sometimes you just suffered or died until a venerble specialist in his white coat opened up his office or started rounds on Monday. Outside of that it was just tough luck.
But it isn’t that way. Death, illness and injury stalk our frantic, frenetic culture around the clock and every day of the week. And the ER is tasked by federal law with providing a ‘safety net.’ But the net has bigger holes and tears at some times than others.
The professionals and ancillary staff members who work nights and weekends find themselves beaten down with hopelessness as patients can’t be seen, admitted or transferred. And the best part is that on Monday morning, someone works tacking billing or safety or some other metric, someone who had the weekend or night to rest, will come along and wonder why people waited so long, or why that important community member was upset about his mother not being admitted to a regular hospital bed. A medication may have take too long to be given, or a bad outcome may have occur.
But none of those things would be suprising to any administrator who spent a few nights in the madness of the emergency department, especially on a busy weekend night when everything was falling apart with fewer staff, fewer resourcds and higher levels of chaos.
The healthcare universe has been changing for decades, and it changed abruptly and violently during COVID. It continues to evolve. But not in a way that offers more for the patient or more support for the clinician.
And few things illustrate that like the way things happen after the sun goes down, and over the hallowed hours of the weekend. Or, heaven help you, a holiday.
I say this as a caution for everyone. The hospital, at night, on the weekend or on a holiday, is not exactly the same as it is other times.
And I say this to those who plan, manage and staff our hospitals.
We can do better. Especially for the price we ask our patients to pay.
Edwin
This is the column on rural vs urban care:


You just spelled out why I was VERY eager and thankful when our daughter asked if I would be their babysitter for my granddaughter. After twelve long years in our transfer center at the institution where I worked for 39 and a half years, I was OVER it. My husband had begged me to quit for 2 years because he was concerned for my mental health. The final straw for me was when administrators decided that my department was NOT getting things done the way they wanted, created a more toxic environment and shifted demands on our workflow. At least 7 nurses (myself included) out of a staff of 15 for 24/7 coverage resigned within 8 months of the hiring of a non nurse manager who had NO clue about the process. (At least 3 more left after I did). No idea how many staff they have now and don't want to know.
Meanwhile staff nurses voted to unionize. I'm not sure that is the answer either, but as an old guard nurse who never thought labor unions had any place in healthcare (we deal with PEOPLE, not airplane or car parts!) I was told I was part of the problem.
So I happily chase my granddaughter and pray I can be a force for good at least in her life, because healthcare as it currently exists is a poor excuse for what people deserve, and as long as the folks in suits are running it and making money, I don't foresee immediate change.
Administrator seen in the ED at nights, weekends, or holidays? Some people believe unicorns exist.
I was fired from my longest ED position, 15 years, because I told an attending that his patient, in the waiting room, couldn’t be seen with her non-urgent problem, right away, because every bed was filled, the hallways were filled with stretchers, and we didn’t have room. Oh, and there were five ambulances outside waiting to offload their patients. The president of the hospital fired me the next day. I guess in Russia, the charge would have been revealing state secrets.